|
By Jyotsna Singh – December
31, 2014
Rat poison theory offered by the Chhattisgarh government to explain the
sterilisation deaths is a facade, finds an investigation by Jyotsna Singh.
The deaths have exposed deep flaws in India's approach to family planning.
As the news of the deaths of women sterilised at a camp at Takhatpur block of
Bilaspur district started to filter in on November 10, officers in
Chhattisgarh's health department pro-actively called all the 83 women present
at the camp to hospitals in the district headquarters. Then, news came that
women who had attended other camps too were feeling unwell. Within hours, the
operation to gather all the 137 women who were sterilised in four camps-one
on November 8 at Nemi Chand Jain hospital in Sikri, Takhatpur, and three on
November 10 in Gaurella block-was initiated. (See `How the tragedy
unfolded').
Once the women's health stabilised, they were sent home with a bag of goodies
that included a shawl, blanket, saree, salt and a kit of toiletries for their
babies. The administration began brainstorming the cause of deaths. It sought
the list of medicines given to the women post-surgery in all four camps. Four
drugs were common in the list-diazepam, ibuprofen, ciprofloxacin and povidine
iodine. Looking at the symptoms of the affected women, they zeroed in on two
drugs, namely ibuprofen and ciprofloxacin. Of these, ibuprofen tablets were
manufactured in 2013 and were in circulation for some time and, therefore,
considered safe.
Survivors of the tubectomies recuperating in a Bilaspur
hospital
How the
tragedy unfolded
An account of what happened in Takhatpur from November 8 onwards
November
8
·
First camp held at Takhatpur. Eighty-three
women sterilised
November 10
·
Three camps at Gaurella, Marwahi and Pendra
villages. Fifty-four women sterilised
·
The first death occurs. Six women taken ill
·
Compensation of Rs 2 lakh for the deceased
November 11
·
Seven more women die
·
R K Gupta, surgeon who operated upon women in
Takhatpur, arrested by police
·
Compensation increased to Rs 4 lakh for the
deceased and Rs 50,000 for survivors
November 12
·
Three more women die
November 13
·
Two more die, one from Pendra town
·
Medicines come under scanner
November 14
·
One-member judicial commission under retired
judge Anita Jha appointed
November 15
·
Zinc phosphide found in ciprofloxacin
·
MahawarPharma promoters arrested
November 18
·
Private Delhi laboratory confirms presence of
zinc phosphide in medicines
·
Fixed deposit of Rs 2 lakh announced for each
child of the deceased
"We found that ciprofloxacin, on the other hand, was manufactured in
October 2014. This made us suspicious and we tested it," said Ayyaj
Fakirbhai Tamboli, mission director, National Rural Health Mission (NRHM),
Chhattisgarh. Preliminary tests of ciprofloxacin tablets showed they were
contaminated by zinc phosphide, commonly used as a rodent killer. The state
government says the labs in Delhi, Nagpur and Kolkata have confirmed the
presence of rat poison but it has not made the reports public. The owners of
Raipur-based Mahawar Pharmaceutical Private Limited and Bilaspur-based Kavita
Pharma were arrested for culpable homicide.
The culprit had been found. The poison that killed the women had been
discovered. Or so it seemed.
A
COVER-UP?
Dularin Patel, 27, of Lokhandi
village in Takhatpur was one of the 13 women who died. "She was fine
till Monday afternoon when she visited us. She had taken medicines on
Saturday night and twice on Sunday," says Gorabai, Dularin's mother.
"She started vomiting from 4 o' clock in the evening. Then, we got a
call from her in-laws, who stay 70 km away, that the mitanin (local health
worker) has asked her to go to the hospital. By 3 o'clock on Tuesday morning,
she was in Chhattisgarh Institute of Medical Sciences (CIMS)."
"I fed my daughter black tea and bread toast before she left home. I did
not know that was going to be her last meal," says Dularin's mother, not
being able to contain tears in her eyes. By early evening on Tuesday, Dularin
was declared dead.
Ranjeeta Suryavanshi of Nirtu village in Takhatpur block died on the
night of November 10. Her husband said he was not given the post-mortem report
despite asking the doctor. Her one-month-old child has no option but to live
on powdered milk (Photographs: Jyotsna Singh)Preliminary results of the
post-mortems of the victims have been submitted to the investigating
agencies. They have not been disclosed to the public but a senior medical
officer who closely monitored the post-mortems told Down To Earth (DTE) that
Dularin had developed septicaemia. "She had inflammation of the
peritoneum, the membrane forming the lining of the abdominal cavity. There was
half-a-litre of thick yellowish fluid in her lungs and septic foci was found
in all organs," said the source, requesting not to be named. "This
is a clear-cut case of postoperative infection."
DTE has accessed seven post-mortem reports. Five of these are of women who
died on November 11, one of a November 12 victim and one of November 13. All
five reports from the first day showed infection of the abdomen. The report
from the second day showed high infection in the body. The report from the
third day showed septic shock.
"This shows the infection kept increasing among women who were
sterilised on November 8. The results show definitively that the women got
infection which must have come through unsterilised instruments," says a
forensic expert at Lady Hardinge Medical College in Delhi.
The administration's beautifully crafted story of contaminated medicines
collapses. The women were prescribed one tablet each of two medicines, twice
a day for five days. One of the medicines was the antibiotic ciprofloxacin,
which the administration claimed was contaminated with rat poison, zinc
phosphide.
Zinc phosphide is linked to kidney failure. "We did not get any renal
failure in our post-mortems," informed the source. He said the infected
laparoscope must have been the reason for the deaths.
As the forensic expert in Delhi explains, zinc phosphide poisoning shows up
as ulceration of the gastrointestinal tract. The source confirmed that signs
of this were missing in post-mortems. However, confirmation of poisoning can
only be through viscera report, which is awaited.
The health department's second assertion too falls flat. It said apart from
the women who underwent sterilisation operations, 26 more people fell sick
after consuming the same medicine. Six of them died.DTE accessed the
post-mortem reports of three of the six. "There was no peculiar finding
in their post-mortems. These can only be confirmed after the chemical
analysis of viscera," said the source.
Though the officials claim that medicines are the culprit, they refuse to
provide the details, saying the matter is sub judice. The only information
they are ready to part with is that two laboratories have confirmed that the
medicines were contaminated with zinc phosphide. They would not say what was
the concentration of the contaminant.
Experts do not believe this theory. "According to standard books, an
adult female needs to consume 4.5 g of zinc phosphide to die," says B L
Chaudhary, from the Department of Forensic Medicine and Toxicology at Lady Hardinge
Medical College. The Chhattisgarh administration claims that 500 mg tablets
of the antibiotic were contaminated. For the sake of argument, even if one
assumes that the entire 500 mg was zinc phosphide, a woman would have to
consume nine tablets for the poison to prove fatal. Most women started to
complain from Monday. By this time, they had taken three to five doses of the
antibiotic. This casts doubt on the poisoning argument.
Citing some of these gaps, this reporter asked the officials about an alternative
line of investigation. "This seems quite conclusive to us. We are not
looking at any other theory. The rest, the lab reports and other tests will
tell," said Tamboli of NRHM.
The state government has set up a one-member judicial commission to
investigate the deaths. It has to collect testimonies of the survivors. But
the commission seems to have placed the responsibility of reporting
grievances on the survivors. People wishing to give testimony will have to
visit the commission's office in Bilaspur city which remains closed most of
the time. "It is impossible to understand how the poor, uneducated and
sick women will travel to this place," says Sulakshana Nandi,
Raipur-based member of Jan Swasthya Abhiyan, the India chapter of People's
Health Movement.
The Bilaspur fiasco has also exposed irregularities in drug procurement. The
much-maligned ciprofloxacin was purchased locally by Chief Medical and Health
Officer (CMHO) R K Bhange. An official in the health department informed DTE
that Chhattisgarh Medical Services Corporation Limited (CGMSCL) has written
to at least one inquiry team, stating that the antibiotic stock was available
with the authority on November 8.
"The CMHO has the discretion to buy medicines or procure from CGMSCL.
Following good practice, he should have chosen the government agency, where
the tenders are invited from companies that have been certified by accredited
labs," said the official.
"It was a double whammy for the women. The tragedy happened due to
multiple reasons. Firstly, the operations were conducted in pathetic and
absolutely unsafe conditions, leaving the women medically vulnerable. Then
they were fed contaminated medicines," says T Sundararaman, founding
director, Chhattisgarh State Health Resource Centre and faculty, Jawaharlal
Nehru University (JNU), Delhi. "All these factors should be investigated
by an independent team. The state should be held responsible for bungling on
all the fronts."
Things
don't change
The manner in which the operations were conducted paints a
disturbing picture. It resembles a scene straight out of the documentary on
sterilisation, Something Like a War, by Bengaluru-based filmmaker
DeepaDhanraj, where a gynaecologist boasts:
This year, I have done more than 2,000 operations. I could do these in school
classes, college rooms and zilaparishad halls. These operations are so easy.
[A woman moans in severe pain in the background.] I thought of this
particular method and I took 45 minutes for the first operation... Now, I can
finish this operation in 45 seconds.
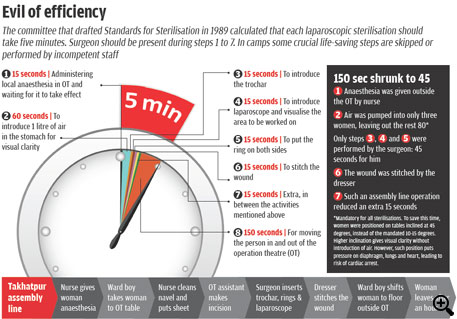
This was 1991. Cut to 2014. Like the gynaecologist in the film, R K Gupta,
operating surgeon at Takhatpur, performed surgeries like an assembly line
(see ‘Evil of efficiency'). He was awarded by the state government on January
26, 2014, for a record 50,000 surgeries in his career.
Accounts of healthcare providers at the Takhatpur camp show gross violation
of the 2006 guidelines, Standards for Female and Male Sterilisation (see
`Flouting of norms on November 8'). Even basic medical ethics went for a
toss. According to the accounts, women started coming to the camp from 10.30
am. Their blood and urine tests were conducted by junior doctors. It was only
at around 3.15 pm that R K Gupta came and he was gone by 5.00 pm after
operating 83 women, giving less than one-and-a-half minutes to each woman.
The same syringe and suture needle were used for all the women. The staff did
not even change their gloves. The hospital floor was just mopped, on which
the operated women lay down in the absence of beds. "This is a sure-shot
recipe for fatal infection. The women could have acquired infection at any
stage," says Subha Sri, member, Common Health, a non-profit working on
maternal and neonatal health.
Accounts of healthcare providers at the Takhatpur camp show gross violation
of the 2006 guidelines, Standards for Female and Male Sterilisation (see
`Flouting of norms on November 8'). Even basic medical ethics went for a
toss. According to the accounts, women started coming to the camp from 10.30
am. Their blood and urine tests were conducted by junior doctors. It was only
at around 3.15 pm that R K Gupta came and he was gone by 5.00 pm after
operating 83 women, giving less than one-and-a-half minutes to each woman.
The same syringe and suture needle were used for all the women. The staff did
not even change their gloves. The hospital floor was just mopped, on which
the operated women lay down in the absence of beds. "This is a sure-shot
recipe for fatal infection. The women could have acquired infection at any
stage," says Subha Sri, member, Common Health, a non-profit working on
maternal and neonatal health.
Flouting of norms on November 8
What happened at the camps and what should have happened
Event at the camps
83 women sterilised
One doctor sterilised them all
Each woman sterilised in one to one-and-a-half minutes
One laparoscope used
No woman knew of the side effects
Nemi Chand Jain hospital was shut since April
No woman knew of other methods of avoiding pregnancy
Operation theatre was cleaned with a mop
Guidelines of 2006
Only 30 persons to be sterlised in one camp
One doctor cansterlise only 10 in a day
Prescribed standards would take an average of 5-6 minutes per case
Three laparoscopes to be used for a maximum of 30 patients
Women should be counselled about side effects
Camp should be conducted in a working hospital
Women have to be counselled about contraceptives and IUDs
The operation theatre should be fumigated thoroughly by burning formaldehyde
tablets and liquid ammonia 48 hours before the surgery
Fatal
planning
India has always leaned heavily
on sterilisation, neglecting other methods of birth control
Although contraceptive pills are advertised on house walls in Lokhandi
village, few women are aware of these options.
On being asked if she knows about spacing methods like intra uterine device
(IUD) or contraceptive pills, Takhatpur survivor Rina Patel answered in the
negative. She also said that no one counselled her at the camp about side
effects and post-operation precautions after sterilisation. (See
‘Sterilisation overdrive'.)
Overemphasis on sterilisation has its roots in the policy followed by India
since 1952 when it became the first nation to adopt an official family
planning programme. A United Nations Advisory Mission visited India in 1965
and persuaded the government to fix targets for widespread use of IUDs. The
next year, the government set up a department of family planning within the
health ministry. While IUDs did not become popular, India embarked on a
target-driven, camp-based approach. Incentives in the form of money and goods
like transistors were offered to sterilisation candidates.
The first camp was organised in 1970 in Ernakulam, Kerala, for vasectomies.
Other parts of the country followed and in 1970-71, nearly 1.3 million
vasectomies took place in India. During Emergency, scores of men were coerced
into vasectomy. Addressing the joint conference of the Association of
Physicians in India in January 1976, then prime minister Indira Gandhi said,
"We must now act decisively and bring down the birth rate...Some
personal rights have to be held in abeyance for the human rights of the
nation." Nearly 6.5 million men were sterilised by the end of 1977.
Gandhi had to pay a price after 1,774 sterilisation-related deaths and her
party lost the elections after the Emergency. "The lesson learnt was:
don't touch the men. And then, the focus shifted to women," says Mohan
Rao, professor of public health at Jawaharlal Nehru University in Delhi.
The department of family planning was also renamed department of family
welfare to make it sound more agreeable. Following a spurt in female
sterilisations and irregularities in operations, the ministry issued
guidelines for sterilisation. By the late 1990s the expenditure on family planning
overtook the health budget (see ‘Skewed Investment'). "It is a lopsided
priority," says Rao. "Better health will help control birth rates,
too. Healthier people, especially children, will mean low infant mortality
rate, encouraging people to reproduce less."
The National Population Policy of 2000 discouraged targets. But in reality it
is targets that hold sway. The target for Takhatpur block, which has 39
sub-centres, for 2014-15 was 2,121 sterilisations, including 1,800 women,
explains Poonam Muttreja, executive director of the national non-profit,
Population Foundation of India, that recently released a fact-finding report
on the Bilaspur deaths. It was further divided among local health workers, so
the average target for female sterilisation per worker was 46.

By the time each state's budget is decided under National Rural Health
Mission (NRHM) and the money reaches the block, half the year is lost. As a
result, most of the camps are crammed into a narrow period of October to
February. The camp approach is being questioned after the Bilaspur tragedy in
the new guidelines on sterilisations to be released in 2015.
Incentives continue to be the norm. A letter by NRHM issued in October says
that family planning is crucial to meet Millennium Development Goals. Citing
the Family Planning 2020 document, it explains that the recently computed
global goals also underline the importance of sterilisation in family
planning. It, thus, revised compensation for sterilisationfrom Rs 600 to Rs
1,400 for each sterilisation candidate, and from Rs 75 to Rs 150 for the
surgeon. The budget for each sterilisation was doubled from Rs 1,000 to Rs
2,000. The revision made tubectomy a lucrative option for surgeons, luring
them into the number game.
The
role of foreign agencies
International agencies
too have played a role in shaping India's policy. In 1952, international
agency Ford Foundation gave $9 million to India for family planning. When
Indira Gandhi spoke of national rights over personal rights, she was under instructions
from the World Bank to bring down India's population growth if the country
wanted food for its hungry.
From 2007-2012, India's family planning was primarily funded by USAID, World
Bank and Department for International Development of the UK government. They
contributed $1 billion. The funding came under attack in 2012, after
sterilised women of a camp in Bihar's Araria district complained to the
police of irregularities. At present, family planning is funded only by the
Indian Government.
But international agencies continue to influence policies of the developing
world. In November this year, pharma major Pfizer and non-profits Bill &
Melinda Gates Foundation (BMGF) and Children's Investment Fund Foundation
announced expansion plans for injectable contraceptive, Sayana Press. This is
part of BMGF's $1 billion project on population control. Sayana Press is made
of the same chemical as Depo Provera, medroxyprogesterone acetate. Depo
Provera has been criticised for adverse health impacts. "Side-effects of
Depo Provera include heavy bleeding, amenorrhoea, depression, weight gain,
breast tenderness, bone thinning, liver damage and cancers," says Subha
Sri of Common Health.
BMGF is sponsoring trials in Africa to see if it is practical for women to inject
themselves. "This makes it scarier. If self-administered, the hazards
include increased chances of HIV transmission," says Sri. Though India
has not yet been mentioned by Sayana Press's promoters, it is a matter of
time before the discussions begin, experts think.
Analysts believe the reasons for international agencies' interest in
developing countries' populations are much deeper. "Population policies
shift the blame for poverty, climate change and food crises on to the poor
and suggest that existing development models which benefit corporate capital
and which are intensifying poverty and inequality don't need to be
changed," says Kalpana Wilson, who teaches at the Gender Institute,
London School of Economics.
Time
for a change
The
Bilaspur tragedy calls for an overhaul of policy on reproductive health
Since the the tragedy in Chhattisgarh, doctors, policy-makers and public
health experts have been trying to find ways to avoid a repeat. A team of
doctors from AIIMS in Delhi went to Bilaspur to help the doctors there
provide the best treatment to the ailing women. Teams of non-governmental
organisations too went on fact-finding missions. The state government has
set-up a judicial inquiry, as well as a health department probe while police
investigates the case. While the probe reports are yet to be released, public
health experts and other concerned people have suggested some short-term and
long-term solutions.
Asking for the operations to be shifted from camps to proper health
facilities, Brinda Karat, former member of Parliament and a prominent voice
on women's issues, said, "The choice of whether to reproduce, method of
birth-control and time should rest with the individual. Sterilisation as an
individual's choice has to be provided in a proper health facility through
the year."
Consensus among the experts is that in the long-term India needs a thorough
review and overhauling of its family planning programme. An overwhelming
demand is to stop using monetary incentives to attract people to unsafe family
planning practices. Target-based sterilisation must end. Instead of camps,
family planning programmes should be available as part of regular healthcare
services. It has to be ensured that women alone are not targeted for
sterlisation and a basket of contraceptive methods is made available to
families. They demand that the women in Bilaspur be provided justice and
their healthcare needs be met. They also suggest that government doctors be
trained to carry out such surgeries safely. In the light of the alleged role
of contaminated medicine, experts suggest that drug procurement policies
should also be reviewed.
It is being pointed out that the rate of population growth in India has now
decreased and the anxiety for speedy population control must stop. According
to census of India, the decadal population growth from 2001-11 came down to
17.6 per cent. It remained above 21 per cent for the preceeding five decades.
"There is a concept called population momentum. It means that population
is growing because of a large number of people in the reproductive age group.
So, even if they have two to three children only, population growth will be
high. We can't do anything about it," Rao says. Around 60 per cent of
the population growth today is due to population momentum, 20 per cent due to
unmet demand of family planning services and 20 per cent is due to unwanted
reproduction, according to a Planning Commission report. Still, India
continues to spend a large part of its population control budget on
sterilisation (see ‘India's lopsided approach').
This
iterates the need to give up the camp approach to family planning. "The
goalpost of the family planning debate has shifted. Now women themselves seek
family planning services. They do not want more than two-three children. We
have to see to it that their demand is met," says T Sundararaman,
founding director, Chhattisgarh State Health Research Centre. Integrating
family planning with the rest of the public system would remove the need for
incentives to meet targets. "We do not need separate camps. The
government can fix one day a week when a laparoscopic surgeon would be
present for sterilisation," he says.
The main challenge is shortage of trained surgeons. "Bilaspur has two
surgeons in the district hospital who are trained in laparoscopy. These
surgeons perform other surgeries too. How can we start a weekly
service?" asks S K Nanda, superintendent, Bilaspur District Hospital. To
this, Sundararaman suggests training more doctors.
Alok Banerjee, member of technical committee on family planning of Government
of India, says that minilaptubectomy should be encouraged. "It is a
simple and inexpensive procedure. While laparoscopy requires high competency,
this can be learnt faster. Also, equipments for minilaptubectomy cost a few
thousand rupees, while one laparascope costs Rs 10 lakh. Its success rate is
also higher. It is not promoted because even a trained surgeon would take
10-15 minutes to perform one surgery. But it is time we cared for meeting
demands and providing safe operations than rushing to sterilise more
people," he says.
Jashodhara Dasgupta, convenor of National Alliance for Maternal Health and
Human Rights, says it is disappointing that India has not been able to
provide basic human rights to women. A pledge to ensure this was taken 20
years ago. In 1994, at the UN conference on population and development held
in Cairo, a 20-year action plan was adopted. This action plan asked countries
to consider women's needs instead of blindly following demographic demands
when planning population control strategies.
Basket of different options for sterilisation also includes male
sterilisation which does not receive any focus. Apart from the fact that
women are seen as easy target for motivation to sterilise, awareness is also
an issue. "Vasectomy is surrounded by many myths like impotency.
Government should create awareness and motivate more men to opt for it,"
says Sri.
A report by a fact-finding mission says that the tragedy in Chhattisgarh was
waiting to happen. In 1974, Karan Singh, the then health minister had
declared: "development is the best contraceptive". This was ignored
at that time. The time has now come to understand this basic concept.
`Phase
out the camps'
Alok Banerjee is a member
of the technical committee that is redrafting the 2006 guidelines on family
planning, and spoke to Down To Earth about the impact of the deaths. Excerpts
What challenges does India face in family planning?
There is non-adherence to national standards and guidelines. The camp sites
are not cleaned properly, patients are not screened by surgeons and many
other violations are rampant. Quality of drugs, their procurement, storage
and supply are also compromised.
Would the Bilaspur deaths impact the new family planning guidelines?
Indeed. Earlier, the new revised guidelines were to be released on November
18-19. Now, they would be released in 2015. According to the proposed
guidelines, doctors are to be trained for sterilisation at MBBS level. More
emphasis is to be put on spacing methods. Having a counsellor at district
hospitals and community health centres would be made mandatory.
Did your Bilaspur visit force a rethink on any suggestions you were
planning to recommend in the committee?
I will see to it that strong emphasis is placed on phasing out the camps.
Also, I will ensure more focus on minilaptubectomy.
What is the way forward?
If we can successfully implement the position of counsellor in public health
facilities and ensure proper follow-up care, then long acting hormonal
methods like injectables, implants and vaginal rings can be introduced. In
any case, spacing methods have to be widely promoted.
________________________________________________________________________________________________________________________________________________________________________________
|

